Flat Feet and Plantar Fasciitis: What’s the Connection?
Why Flat Feet Can Lead to Plantar Fasciitis
If you’ve been waking up with sharp heel pain or feeling discomfort after long hours on your feet, you’re not alone. One of the most common—but often overlooked—connections in foot health is the link between flat feet and plantar fasciitis.
At first glance, they might seem like separate issues. One relates to foot structure, the other to inflammation. But in reality, they are closely connected through biomechanics—how your body moves and absorbs stress.
Understanding this relationship is key to addressing the root cause rather than just managing symptoms.
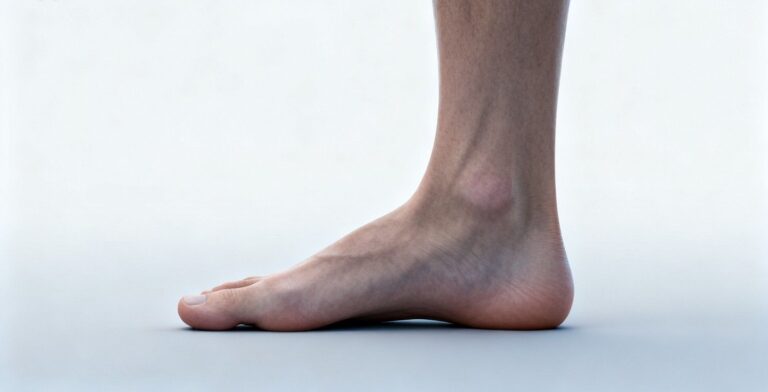
What Are Flat Feet?
Flat feet, also known as fallen arches, occur when the arch of the foot collapses or remains very low. Instead of distributing weight efficiently, the entire sole of the foot makes contact with the ground.
This changes how force moves through your body.
Normally, the arch acts like a spring:
- It absorbs impact
- It stabilizes movement
- It distributes pressure
With flat feet:
- The arch doesn’t absorb shock effectively
- The foot rolls inward excessively (overpronation)
- Pressure shifts to areas not designed to handle it
Over time, this altered movement pattern creates stress in the foot—especially in the plantar fascia.
What Is Plantar Fasciitis?
Plantar fasciitis is a condition involving inflammation of the plantar fascia, a thick band of tissue that runs along the bottom of your foot—from the heel to the toes.
This tissue:
- Supports the arch
- Helps absorb shock
- Plays a key role in walking mechanics
When it becomes irritated or overloaded, it leads to:
- Sharp heel pain (especially in the morning)
- Stiffness after rest
- Pain that worsens with activity
How Flat Feet Cause Plantar Fasciitis
The connection between flat feet and plantar fasciitis comes down to repeated strain.
When your arch collapses:
- The plantar fascia stretches more than it should
- The foot loses structural support
- The fascia is forced to compensate
This constant overstretching creates micro-tears in the tissue. Over time, inflammation develops—and that’s when pain begins.
People with flat feet often experience:
- Increased tension along the bottom of the foot
- Reduced shock absorption
- Poor alignment through the ankle and leg
This is why many individuals dealing with flat feet eventually develop plantar fasciitis if the underlying issue isn’t addressed.
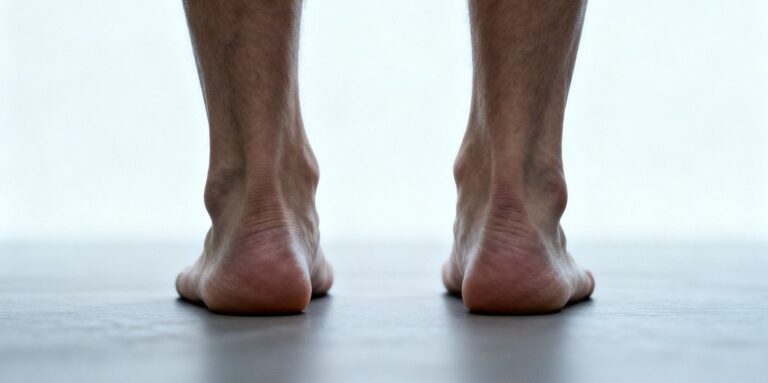
The Role of Overpronation
Flat feet are strongly associated with overpronation, where the foot rolls inward excessively during movement.
This inward motion:
- Increases strain on the plantar fascia
- Changes how force travels through the foot
- Reduces stability during walking or running
For a deeper understanding of how alignment affects foot mechanics, see flat feet vs overpronation differences.
Over time, this repetitive movement pattern places continuous stress on the fascia, especially during high-impact activities or long periods of standing.
Risk Factors That Make It Worse
Not everyone with flat feet develops plantar fasciitis—but certain factors increase the likelihood.
1. Long Hours Standing or Walking
Jobs that require prolonged standing can overload the plantar fascia, especially without proper support.
2. Improper Footwear
Shoes that lack arch support or stability allow the foot to collapse further, increasing strain.
3. Sudden Increase in Activity
Jumping into running or exercise without proper conditioning puts additional stress on the foot.
4. Body Weight
Higher body weight increases pressure on the arch and plantar fascia.
5. Tight Muscles
Tight calves or Achilles tendons can pull on the heel, adding tension to the plantar fascia.
How Symptoms Differ Between the Two
Although related, flat feet and plantar fasciitis present differently.
Flat Feet Symptoms:
- Foot fatigue
- Arch discomfort
- Inward ankle movement
- General instability
Plantar Fasciitis Symptoms:
- Sharp heel pain (especially in the morning)
- Pain after rest
- Tenderness under the heel
- Pain that improves slightly with movement
When It Becomes Serious
The combination of flat feet and plantar fasciitis can worsen over time if ignored.
Warning signs include:
- Persistent pain lasting weeks
- Difficulty walking normally
- Pain spreading to knees or hips
- Reduced mobility
At this stage, your body is no longer compensating effectively—the stress has exceeded what your tissues can handle.
The Bigger Picture
So, how are flat feet and plantar fasciitis connected?
Flat feet change how your foot absorbs impact and maintains alignment. This increases strain on the plantar fascia, which eventually leads to inflammation and pain.
It’s not just a foot issue—it’s a movement issue.
Understanding that connection is the first step toward fixing it properly.
How to Treat, Support, and Prevent Flat Feet–Related Plantar Fasciitis
Understanding the connection between flat feet and plantar fasciitis gives you a clear advantage—you’re no longer just treating symptoms, you’re addressing the root cause.
Now the focus shifts to what actually helps.
There’s no single fix, but there is a structured approach that consistently works when applied correctly.
Non-Commercial Treatment Options (Start Here First)
Before considering insoles or other support tools, it’s important to reduce stress on the plantar fascia and allow the tissue to recover.
1. Reduce Load and Impact
If you’re dealing with active pain, your first priority is lowering stress on the foot.
That means:
- Avoiding high-impact activity (running, jumping)
- Limiting long periods of standing
- Switching to low-impact movement (cycling, swimming)
This gives the inflamed tissue time to calm down.
2. Stretch the Right Structures
Tight muscles often contribute to plantar fasciitis.
Focus on:
- Calf muscles (gastrocnemius and soleus)
- Achilles tendon
- Plantar fascia itself
Regular stretching improves flexibility and reduces tension on the heel.
3. Strengthen Foot and Lower Leg Muscles
Flat feet often come with weak stabilizing muscles.
Strengthening helps:
- Support the arch naturally
- Improve alignment
- Reduce reliance on passive structures like the fascia
Simple exercises include:
- Toe curls
- Heel raises
- Arch lifts
Over time, these help your foot handle stress more efficiently.
4. Improve Daily Movement Habits
Small adjustments matter more than people think.
- Avoid walking barefoot on hard floors
- Rotate shoes instead of using the same pair daily
- Pay attention to posture and walking pattern
Consistency here reduces long-term strain.
When Insoles Actually Help
Insoles can play a significant role—but only when used correctly.
They are most effective when:
- Flat feet are contributing to poor alignment
- The arch needs structural support
- Pain is linked to repetitive stress
By supporting the arch and stabilizing the foot, insoles:
- Reduce strain on the plantar fascia
- Improve weight distribution
- Limit excessive inward motion
For people dealing with alignment-related issues, structured support like best insoles for overpronation can help control movement and reduce stress on the foot.
Matching Support to Your Needs
Not all insoles work the same way.
- Mild discomfort → moderate support + cushioning
- Chronic pain → firmer, structured support
- High activity → stability + shock absorption
Flat feet often benefit from solutions similar to those explained in insoles for flat feet, where arch support and control are prioritized over softness.
When Medical Care Is Required
While many cases improve with proper support and adjustments, some situations require professional evaluation.
You should seek medical advice if:
- Pain persists beyond a few weeks
- Symptoms worsen despite rest
- You experience sharp or localized heel pain
- Walking becomes difficult
A healthcare professional may recommend:
- Physical therapy
- Custom orthotics
- Imaging if necessary
Early intervention can prevent long-term complications.
Prevention: How to Stop It from Coming Back
Once you understand how flat feet plantar fasciitis develops, prevention becomes much easier.
1. Maintain Arch Support
Whether through footwear or insoles, consistent support helps reduce strain on the plantar fascia.
2. Build Strength Over Time
Strong muscles reduce dependency on passive structures.
Regular foot and leg exercises make a noticeable difference.
3. Avoid Sudden Activity Changes
Gradual progression allows your body to adapt without overload.
4. Replace Worn-Out Support
Shoes and insoles lose effectiveness over time.
If support breaks down, stress increases again.
If you’re unsure when to replace them, see signs you need new insoles for guidance.
5. Stay Consistent
The biggest factor isn’t intensity—it’s consistency.
Small, daily habits prevent long-term problems.
Frequently Asked Questions
Can flat feet directly cause plantar fasciitis?
Yes. Flat feet increase strain on the plantar fascia due to poor arch support and excessive inward motion.
Do insoles fix plantar fasciitis permanently?
They help manage the condition by reducing stress, but they don’t permanently change foot structure.
How long does recovery take?
Mild cases may improve within a few weeks, while more persistent cases can take several months depending on treatment and activity level.
Is walking good or bad for plantar fasciitis?
Moderate walking is usually fine, but excessive walking—especially without support—can worsen symptoms.
Are custom orthotics necessary?
Not always. Many people benefit from well-designed over-the-counter support unless the condition is severe.
You can explore our in-depth foot care guides here for more.
Final Thoughts: Fix the Cause, Not Just the Pain
Flat feet and plantar fasciitis are deeply connected through movement and alignment.
When the arch collapses, the plantar fascia is forced to absorb more stress than it should. Over time, that leads to inflammation, discomfort, and reduced mobility.
The solution isn’t just rest—or just support.
It’s a combination of:
- Better movement
- Proper support
- Consistent prevention
When you address the underlying mechanics, you don’t just reduce pain—you restore function.